(54) High Dose Buprenorphine Induction Precipitating Non-Cardiogenic Pulmonary Edema
Friday, April 5, 2024
9:45 AM - 1:15 PM
Has Audio

Daniel Liauw, MD, MPH
Addiction Medicine Fellow
Massachusetts General Hospital, Program in Substance Use & Addiction Services, Massachusetts
Evan Gale, MD, FASAM
Associate Medical Director
MGH Addiction Consult Team, Massachusetts
Presenter(s)
Background & Introduction: In the era of high-potency synthetic opioids, there has been growing interest in the high-dose buprenorphine initiation (HDBI) protocol, as explored in American Society of Addiction Medicine’s recent review of buprenorphine clinical considerations [1,2]. This approach utilizes buprenorphine’s increased mu-opioid receptor activation at high doses (beyond 8mg sublingual) to provide relief of withdrawal symptoms. However, data supporting the safety and efficacy of HDBI remains limited. Here, we present a case where a HDBI protocol precipitated withdrawal and culminated in severe respiratory distress requiring intubation.
Case Description: JJ is a 52yo caregiver with a history of severe OUD (previously on buprenorphine and methadone, 10g intranasal and injection use daily), moderate benzodiazepine use disorder (4-5mg non-prescribed clonazepam daily), and mild COPD who was admitted for a fever to 105F in the context of injection fentanyl use.
JJ’s goals were to achieve recovery through a transition to buprenorphine and to return home quickly to care for her partner. She previously sustained OUD remission while on buprenorphine and strongly preferred avoiding methadone, even for a time-limited period for withdrawal management. She feared precipitated withdrawal but also worried that temporarily feeling well enough on methadone might prompt a self-directed discharge. Inflexibility of methadone dosing had previously interfered with her caregiving capacity.
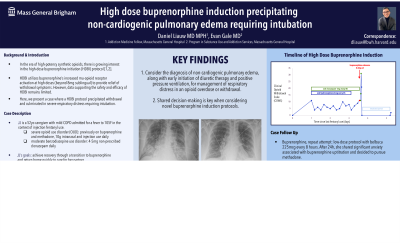
Thus, we held a PARQ (Procedure, Alternative, Risk, Question) conference and pursued a high-dose buprenorphine induction with JJ’s informed consent. With last fentanyl use 24h prior to presentation, JJ was bridged with scheduled hydromorphone 6mg every 3h for 51h, during which she experienced mild opioid withdrawal (Clinical Opioid Withdrawal Scale, COWS: 4-11). Throughout the washout period, her most significant symptom was anxiety, managed with clonazepam 1mg every 8h. This was followed by a 11.5h period without full or partial opioid agonists, representing 86.5hrs since last fentanyl use. With a COWS of 11, she received three, buprenorphine-naloxone 8-2mg films, each a minute apart, along with clonazepam 2mg. Her COWS was 16 (1hr later) then 31 (2hrs later with severe respiratory distress). With a respiratory rate of 40 and oxygen saturation of 70% on maximal bilevel positive airway pressure settings, she was intubated. Physical exam was notable for flat neck veins and lack of peripheral edema.
Chest X-ray, compared to admission, demonstrated new pulmonary edema with pleural effusions, and trans-thoracic echocardiography was without evidence of systolic or diastolic dysfunction. With mild diuresis, oxygen requirements were quickly weaned, and she was extubated to room air within 48h. The respiratory failure was attributed to non-cardiogenic pulmonary edema in the setting of precipitated withdrawal following HDBI. With a negative broad infectious work-up, the fever was attributed to cotton fever.
Following extubation, JJ re-attempted buprenorphine with a low-dose protocol using belbuca 225mcg every 8 hours. After 24h, she shared significant anxiety associated with buprenorphine uptitration and decided to pursue methadone. She received methadone 80mg on day 1 and 100mg on day 2. On day 3, she was discharged to an opioid treatment program on methadone 100mg daily.
Conclusion & Discussion: This case highlights a rare, adverse reaction of HDBI: non-cardiogenic pulmonary edema. Pulmonary edema has been associated with a majority of fatal opioid overdoses [3]. Non-cardiogenic pulmonary edema has been associated with heroin and naloxone, each with incompletely defined pathophysiology [4,5]. Naloxone is proposed to trigger an adrenergic crisis, increasing pulmonary vasculature permeability; this mechanism might be presumed of HDBI-associated precipitated withdrawal. While more specific imaging such as a cardiac MRI is needed to definitively exclude a HFpEF diagnosis, echocardiography did not suggest a cardiac cause of fulminant pulmonary edema.
Clinicians ought to consider the diagnosis of non-cardiogenic pulmonary edema, along with early initiation of diuretic therapy and positive pressure ventilation, for management of respiratory distress in the setting of opioid overdose or precipitated withdrawal. For patients with high opioid tolerance, an extended washout period might be warranted prior to consideration of HDBI.
This case also raises the need for caution and shared decision-making when considering novel buprenorphine induction protocols. The patient’s strong preference for an expedited transition to buprenorphine and equally strong fear of precipitated withdrawal from prior traditional induction attempts suggested benefit from a HDBI protocol, in lieu of traditional and low-dose buprenorphine induction protocols.
References:
1. Herring, A. A., Vosooghi, A. A., Luftig, J., Anderson, E. S., Zhao, X., Dziura, J., … D’Onofrio, G. (2021). High-dose buprenorphine induction in the emergency department for treatment of opioid use disorder. JAMA Network Open, 4(7), e2117128. doi:10.1001/jamanetworkopen.2021.17128
2. Weimer, M. B., Herring, A. A., Kawasaki, S. S., Meyer, M., Kleykamp, B. A., & Ramsey, K. S. (2023). ASAM clinical considerations: Buprenorphine treatment of opioid use disorder for individuals using high-potency synthetic opioids. Journal of Addiction Medicine. doi:10.1097/ADM.0000000000001202
3. Winklhofer, S., Surer, E., Ampanozi, G., Ruder, T., Stolzmann, P., Elliott, M., … Schweitzer, W. (2014). Post-mortem whole body computed tomography of opioid (heroin and methadone) fatalities: frequent findings and comparison to autopsy. European Radiology, 24(6), 1276–1282. doi:10.1007/s00330-014-3128-7
4. Farkas, A., Lynch, M. J., Westover, R., Giles, J., Siripong, N., Nalatwad, A., … Martin-Gill, C. (2020). Pulmonary complications of opioid overdose treated with naloxone. Annals of Emergency Medicine, 75(1), 39–48. doi:10.1016/j.annemergmed.2019.04.006
5. Sporer, K. A., & Dorn, E. (2001). Heroin-related noncardiogenic pulmonary edema. Chest, 120(5), 1628–1632. doi:10.1378/chest.120.5.1628
Case Description: JJ is a 52yo caregiver with a history of severe OUD (previously on buprenorphine and methadone, 10g intranasal and injection use daily), moderate benzodiazepine use disorder (4-5mg non-prescribed clonazepam daily), and mild COPD who was admitted for a fever to 105F in the context of injection fentanyl use.
JJ’s goals were to achieve recovery through a transition to buprenorphine and to return home quickly to care for her partner. She previously sustained OUD remission while on buprenorphine and strongly preferred avoiding methadone, even for a time-limited period for withdrawal management. She feared precipitated withdrawal but also worried that temporarily feeling well enough on methadone might prompt a self-directed discharge. Inflexibility of methadone dosing had previously interfered with her caregiving capacity.
Thus, we held a PARQ (Procedure, Alternative, Risk, Question) conference and pursued a high-dose buprenorphine induction with JJ’s informed consent. With last fentanyl use 24h prior to presentation, JJ was bridged with scheduled hydromorphone 6mg every 3h for 51h, during which she experienced mild opioid withdrawal (Clinical Opioid Withdrawal Scale, COWS: 4-11). Throughout the washout period, her most significant symptom was anxiety, managed with clonazepam 1mg every 8h. This was followed by a 11.5h period without full or partial opioid agonists, representing 86.5hrs since last fentanyl use. With a COWS of 11, she received three, buprenorphine-naloxone 8-2mg films, each a minute apart, along with clonazepam 2mg. Her COWS was 16 (1hr later) then 31 (2hrs later with severe respiratory distress). With a respiratory rate of 40 and oxygen saturation of 70% on maximal bilevel positive airway pressure settings, she was intubated. Physical exam was notable for flat neck veins and lack of peripheral edema.
Chest X-ray, compared to admission, demonstrated new pulmonary edema with pleural effusions, and trans-thoracic echocardiography was without evidence of systolic or diastolic dysfunction. With mild diuresis, oxygen requirements were quickly weaned, and she was extubated to room air within 48h. The respiratory failure was attributed to non-cardiogenic pulmonary edema in the setting of precipitated withdrawal following HDBI. With a negative broad infectious work-up, the fever was attributed to cotton fever.
Following extubation, JJ re-attempted buprenorphine with a low-dose protocol using belbuca 225mcg every 8 hours. After 24h, she shared significant anxiety associated with buprenorphine uptitration and decided to pursue methadone. She received methadone 80mg on day 1 and 100mg on day 2. On day 3, she was discharged to an opioid treatment program on methadone 100mg daily.
Conclusion & Discussion: This case highlights a rare, adverse reaction of HDBI: non-cardiogenic pulmonary edema. Pulmonary edema has been associated with a majority of fatal opioid overdoses [3]. Non-cardiogenic pulmonary edema has been associated with heroin and naloxone, each with incompletely defined pathophysiology [4,5]. Naloxone is proposed to trigger an adrenergic crisis, increasing pulmonary vasculature permeability; this mechanism might be presumed of HDBI-associated precipitated withdrawal. While more specific imaging such as a cardiac MRI is needed to definitively exclude a HFpEF diagnosis, echocardiography did not suggest a cardiac cause of fulminant pulmonary edema.
Clinicians ought to consider the diagnosis of non-cardiogenic pulmonary edema, along with early initiation of diuretic therapy and positive pressure ventilation, for management of respiratory distress in the setting of opioid overdose or precipitated withdrawal. For patients with high opioid tolerance, an extended washout period might be warranted prior to consideration of HDBI.
This case also raises the need for caution and shared decision-making when considering novel buprenorphine induction protocols. The patient’s strong preference for an expedited transition to buprenorphine and equally strong fear of precipitated withdrawal from prior traditional induction attempts suggested benefit from a HDBI protocol, in lieu of traditional and low-dose buprenorphine induction protocols.
References:
1. Herring, A. A., Vosooghi, A. A., Luftig, J., Anderson, E. S., Zhao, X., Dziura, J., … D’Onofrio, G. (2021). High-dose buprenorphine induction in the emergency department for treatment of opioid use disorder. JAMA Network Open, 4(7), e2117128. doi:10.1001/jamanetworkopen.2021.17128
2. Weimer, M. B., Herring, A. A., Kawasaki, S. S., Meyer, M., Kleykamp, B. A., & Ramsey, K. S. (2023). ASAM clinical considerations: Buprenorphine treatment of opioid use disorder for individuals using high-potency synthetic opioids. Journal of Addiction Medicine. doi:10.1097/ADM.0000000000001202
3. Winklhofer, S., Surer, E., Ampanozi, G., Ruder, T., Stolzmann, P., Elliott, M., … Schweitzer, W. (2014). Post-mortem whole body computed tomography of opioid (heroin and methadone) fatalities: frequent findings and comparison to autopsy. European Radiology, 24(6), 1276–1282. doi:10.1007/s00330-014-3128-7
4. Farkas, A., Lynch, M. J., Westover, R., Giles, J., Siripong, N., Nalatwad, A., … Martin-Gill, C. (2020). Pulmonary complications of opioid overdose treated with naloxone. Annals of Emergency Medicine, 75(1), 39–48. doi:10.1016/j.annemergmed.2019.04.006
5. Sporer, K. A., & Dorn, E. (2001). Heroin-related noncardiogenic pulmonary edema. Chest, 120(5), 1628–1632. doi:10.1378/chest.120.5.1628
Learning Objectives:
- Highlight a rare but significant adverse outcome of a high-dose buprenorphine induction
- Understand diagnosis and management of non-cardiogenic pulmonary edema in the setting of opioid overdose or precipitated withdrawal
- Discuss a structured approach to incorporating patient perspectives and improving informed consent for novel buprenorphine inductions
