(17) Keeping Patients in Care?: Factors Associated with Patients Returning to Care
Friday, April 5, 2024
9:45 AM - 1:15 PM

Phyllis Losikoff, MD
Medical Dir Research
CleanSlate Centers, Massachusetts- CJ
Claudie Jimenez, MD
Chief Medical Officer
CleanSlate Centers, Tennessee 
Matthew Hanauer, MPA, PhD
Senior Data Scientist
CleanSlate Centers, North Carolina
Presenter(s)
Non-presenting author(s)
Background & Introduction: Retention in treatment with medication for opioid use disorder (MOUD) is associated with better patient outcomes, decreased use of non-prescribed substances, and decreased morbidity and mortality (Bart, 2012). Unfortunately, in most studies, less than half of patients remain in treatment for 6 months or more. (Chan et al., 2021, Kennedy et al., 2021) Moreover, few interventions have successfully improved retention rates MOUD treatment (Chan et al., 2021, Kennedy et al., 2021). Leaving care occurs for many reasons: those associated with the patient’s use disorder, such as returning to drug use and mental or physical health crises or related external factors, such as loss of housing, employment, or transportation and change or loss of health insurance.
While gaps in care may not be avoidable, the desired outcome is to have patients return to care to avoid increased risk of morbidity and mortality.
We aimed to identify factors associated with patients returning to our program after a gap in treatment.
While gaps in care are unavoidable, the desired outcome is to have patients return to care to avoid increased risk of morbidity and mortality.
We aimed to identify factors associated with patients returning to our program after a gap in treatment.
Methods: We performed a cohort study utilizing electronic medical records, including all patients who initiated MOUD treatment at CleanSlate between 7/31/2021 and 7/31/2022. Our outcome was discharged patients (i.e., no medical visits in the past 90 days) who returned to care (i.e., had at least one medical appointment after discharge within a year of their last medical appointment). Patients were followed until 7/31/2023. We identified factors associated with patients returning to care by conducting a repeated cross-validation XGBoost logistic model with Bayesian hyperparameter optimization to identify the best fitting model. We included over 30 features in the initial model. From that model, we calculated Shapley values, which identify the unique contribution of each feature on each patient’s predicted outcome value, similar to parameter estimates in a regression analysis. We present features making the largest contribution to the outcome.
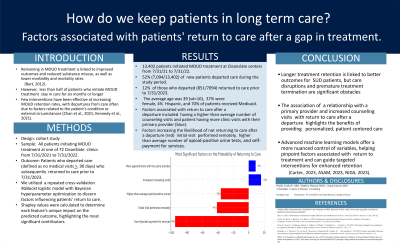
Results: Between 7/31/21 and 7/31/22, 13,402 patients had initial visits, and of those, 7,094 left care for at least 90 days sometime between 7/31/2021 and 7/31/2022 (average age 39, sd = 10, 37% female n = 2,656). Twelve percent of these patients returned to care before 7/31/2023. Of the factors modeled, the more appointments a patient had with their primary provider, the more likely they were to return to care after a gap, increasing the probability of return to care by 9%. Increased counseling visits increased the probability of returning to care by 16%. Factors that negatively impact return to care include patients having an initial visit performed remotely rather than in person, leading to a 41% decrease in the probability of returning to care after a > 90-day gap. Patients with a higher-than-average number of urines positive for opioids were 36% less likely to return to care, and patients who paid out of pocket for services were 95% less likely to return to care after a >90 day gap.
Conclusion & Discussion: Longer retention in treatment is associated with improved outcomes for patients suffering from SUD. Nonetheless, disruptions in care and early disengagement remains a challenge to effective treatment. Notably, our findings show having a relationship with a primary provider and increased exposure to counseling are both associated with return to care after a hiatus point to the importance of individualized care focusing on patients’ specific needs. (Carter et al., 2023, ASAM, 2023, NIDA, 2023). Leveraging advanced machine learning models, which can control for many more factors than traditional modeling, enables us to identify better factors associated with return to treatment and focus resources on targeted interventions to improve long-term retention.
References: American Society of Addiction Medicine. (2020). National Practice Guideline for the Treatment of Opioid Use Disorder. Retrieved September 30, 2023, from https://www.asam.org/quality-care/clinical-guidelines/national-practice-guideline
Bart, G. (2012). Maintenance medication for opiate addiction: the foundation of recovery. Journal of addictive diseases, 31(3), 207-225.
Carter, M., Boyd, J., Bennett, T., & Baus, A. (2023). Medication Assisted Treatment Program Policies: Opinions of People in Treatment. Journal of Primary Care & Community Health, 14, 21501319231195606.
Chan, B., Gean, E., Arkhipova-Jenkins, I., Gilbert, J., Hilgart, J., Fiordalisi, C., ... & Guise, J. M. (2021). Retention strategies for medications for opioid use disorder in adults: a rapid evidence review. Journal of addiction medicine, 15(1), 74.
Kennedy, A. J., Wessel, C. B., Levine, R., Downer, K., Raymond, M., Osakue, D., ... & Liebschutz, J. M. (2022). Factors associated with long-term retention in buprenorphine-based addiction treatment programs: A systematic review. Journal of general internal medicine, 1-9.
National Institute on Drug Abuse; National Institutes of Health; U.S. Department of Health and Human Services. (2018). Principles of Drug Addiction Treatment: A Research-Based Guide (3rd ed.). Retrieved September 30, 2023, from https://nida.nih.gov/sites/default/files/675-principles-ofdrug-addiction-treatment-a-research-based-guide-thir
While gaps in care may not be avoidable, the desired outcome is to have patients return to care to avoid increased risk of morbidity and mortality.
We aimed to identify factors associated with patients returning to our program after a gap in treatment.
While gaps in care are unavoidable, the desired outcome is to have patients return to care to avoid increased risk of morbidity and mortality.
We aimed to identify factors associated with patients returning to our program after a gap in treatment.
Methods: We performed a cohort study utilizing electronic medical records, including all patients who initiated MOUD treatment at CleanSlate between 7/31/2021 and 7/31/2022. Our outcome was discharged patients (i.e., no medical visits in the past 90 days) who returned to care (i.e., had at least one medical appointment after discharge within a year of their last medical appointment). Patients were followed until 7/31/2023. We identified factors associated with patients returning to care by conducting a repeated cross-validation XGBoost logistic model with Bayesian hyperparameter optimization to identify the best fitting model. We included over 30 features in the initial model. From that model, we calculated Shapley values, which identify the unique contribution of each feature on each patient’s predicted outcome value, similar to parameter estimates in a regression analysis. We present features making the largest contribution to the outcome.
Results: Between 7/31/21 and 7/31/22, 13,402 patients had initial visits, and of those, 7,094 left care for at least 90 days sometime between 7/31/2021 and 7/31/2022 (average age 39, sd = 10, 37% female n = 2,656). Twelve percent of these patients returned to care before 7/31/2023. Of the factors modeled, the more appointments a patient had with their primary provider, the more likely they were to return to care after a gap, increasing the probability of return to care by 9%. Increased counseling visits increased the probability of returning to care by 16%. Factors that negatively impact return to care include patients having an initial visit performed remotely rather than in person, leading to a 41% decrease in the probability of returning to care after a > 90-day gap. Patients with a higher-than-average number of urines positive for opioids were 36% less likely to return to care, and patients who paid out of pocket for services were 95% less likely to return to care after a >90 day gap.
Conclusion & Discussion: Longer retention in treatment is associated with improved outcomes for patients suffering from SUD. Nonetheless, disruptions in care and early disengagement remains a challenge to effective treatment. Notably, our findings show having a relationship with a primary provider and increased exposure to counseling are both associated with return to care after a hiatus point to the importance of individualized care focusing on patients’ specific needs. (Carter et al., 2023, ASAM, 2023, NIDA, 2023). Leveraging advanced machine learning models, which can control for many more factors than traditional modeling, enables us to identify better factors associated with return to treatment and focus resources on targeted interventions to improve long-term retention.
References: American Society of Addiction Medicine. (2020). National Practice Guideline for the Treatment of Opioid Use Disorder. Retrieved September 30, 2023, from https://www.asam.org/quality-care/clinical-guidelines/national-practice-guideline
Bart, G. (2012). Maintenance medication for opiate addiction: the foundation of recovery. Journal of addictive diseases, 31(3), 207-225.
Carter, M., Boyd, J., Bennett, T., & Baus, A. (2023). Medication Assisted Treatment Program Policies: Opinions of People in Treatment. Journal of Primary Care & Community Health, 14, 21501319231195606.
Chan, B., Gean, E., Arkhipova-Jenkins, I., Gilbert, J., Hilgart, J., Fiordalisi, C., ... & Guise, J. M. (2021). Retention strategies for medications for opioid use disorder in adults: a rapid evidence review. Journal of addiction medicine, 15(1), 74.
Kennedy, A. J., Wessel, C. B., Levine, R., Downer, K., Raymond, M., Osakue, D., ... & Liebschutz, J. M. (2022). Factors associated with long-term retention in buprenorphine-based addiction treatment programs: A systematic review. Journal of general internal medicine, 1-9.
National Institute on Drug Abuse; National Institutes of Health; U.S. Department of Health and Human Services. (2018). Principles of Drug Addiction Treatment: A Research-Based Guide (3rd ed.). Retrieved September 30, 2023, from https://nida.nih.gov/sites/default/files/675-principles-ofdrug-addiction-treatment-a-research-based-guide-thir
Learning Objectives:
- Understand MOUD Retention Significance: Participants will grasp the importance of patient retention in Medication for Opioid Use Disorder (MOUD) for improved outcomes and decreased morbidity and mortality rates.
- Identify Return-to-Care Factors: Participants will learn key factors affecting patients' return to MOUD care after treatment gaps, including roles of primary care and counseling.
- Explore Advanced Analytical Models: Attendees will understand the utility of machine learning models like XGBoost in identifying nuanced factors that influence MOUD treatment retention.
