(1) Nicotine Use and Patient Directed Discharge Rate in Psychiatric Inpatients
Friday, April 5, 2024
9:45 AM - 1:15 PM
Has Audio

Steven Sprenger, MD
Resident Physician
Tristar centennial Medical Center, Tennessee- OG
Olivia Gawrych, MD
Attending Physician
Tristar Centennial Medical Center, Tennessee
Presenter(s)
Non-presenting author(s)
Background & Introduction: Sequelae of tobacco use disproportionately affects psychiatric patients. Patients with serious mental illness are more than twice as likely to smoke with approximately half of psychiatric inpatients using tobacco. Cessation treatments are underutilized in this population despite tobacco use having a deleterious effect on care by altering the metabolism of many therapeutic drugs, worsening numerous psychiatric symptoms, and interfering with the delivery of care. An important but understudied aspect is the effect of tobacco use on patient directed discharge (PDD) rates. A positive correlation was shown in one study. Another study found patients who smoke were twice as likely to undergo PDD, but nicotine replacement therapy ameliorated this disparity. However, these studies were conducted in limited patient populations from single facilities. The effect of pharmacotherapy on rates has not been replicated. Given the importance of continuity of care in this population, a more thorough understanding of the association is critical. The purpose of this study was to investigate the effect of tobacco use on PDD rate, to determine associated factors, and to investigate how individual forms of tobacco cessation pharmacotherapy attenuate the association.
Methods: A retrospective analysis was conducted using a random sample of adult patients admitted voluntarily to inpatient psychiatric facilities in a nationwide hospital system. Exclusionary criteria included medical discharge, administration of electroconvulsive therapy, hospital stay > 29 days, and patients with indeterminate demographics or smoking status. Demographic variables including age, sex, race, insurance type, and psychiatric diagnosis were assembled. Binary logistic regression with a Firth correction was used to determine associations between patient directed discharge (PDD) rates and smoking status, smoking cessation treatments, demographic variables, comorbidities, and use patterns.
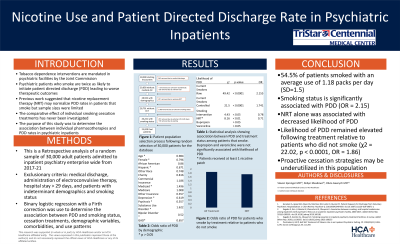
Results: A total of 30,000 patients were randomly sampled resulting in 25,829 patients after the application of exclusionary criteria. The average age in the sample was 41 years (SD=17.3) and 54.5% of patients smoked with an average use of 1.18 packs per day (SD=1.5). Smoking status was significantly associated with the likelihood of PDD (χ2 = 49.42, p < 0.0001, OR = 2.16). This effect was preserved despite controlling for other variables (χ2 = 21.50, p < 0.0001 OR = 1.74). Pharmaceutical intervention overall was associated with a decreased PDD (χ2 = 4.43, p < 0.05 OR = 1.29), however nicotine replacement therapy (NRT) alone had a significant association (χ2 = 8.16, p < 0.01 OR 1.42). Bupropion and varenicline were not associated with significant differences in PDD rates. Rates of PDD remained elevated despite treatment relative to patients who did not smoke (χ2 = 22.02, p < 0.0001, OR = 1.86). Sex (χ2 = 4.77, p < 0.05) was significantly associated with discharge rates while racial identity and insurance type were significant only when comparing Hispanic to White (χ2 = 4.68, p < 0.05) and Medicaid to no insurance (χ2 = 6.41, p < 0.05). Interestingly, use characteristics including packs per day, pack years, use of smokeless tobacco, and use of vapes were not significantly associated with likelihood of PDD (all p > 0.05). Co-occurring substance use disorder (SUD) was associated with elevated risk of PDD (χ2 = 16.76, p < 0.0001, OR 1.62) while diagnoses of depression (χ2 = 17.48, p < 0.0001, OR = 0.62), psychosis (χ2 = 48.98, p < 0.0001, OR = 0.36), and bipolar disorder (χ2 = 22.60, p < 0.0001, OR = 0.52) were associated with decreased risk.
Conclusion & Discussion: This was the largest study of its kind investigating the association between tobacco use and patient directed discharge rates in a national sample of psychiatric patients. The results support previous findings that more than half of psychiatric inpatients report smoking and use of tobacco is associated with increased risk of PDD while providing further insight on the effect of pharmacotherapy. This was the first attempt to investigate the association of PDD with individual treatment modalities. NRT alone was associated with lower PDD rates while bupropion and varenicline were not. Contrary to previous reports, the risk of PDD remained significantly elevated despite treatment. Sex and co-occurring SUD were associated with higher risk while other demographic variables were not. The finding that use characteristics including duration and amount of smoking was not associated with PDD rates is querulous and warrants replication. Tobacco cessation constitutes an important aspect of psychiatric care and consistent use of NRT may attenuate but not normalize the risk of PDD for patients who smoke.
References: 1. Kagabo R, Gordon AJ, Okuyemi K. Smoking cessation in inpatient psychiatry treatment facilities: A review. Addict Behav Rep. 2020;11:100255. doi:10.1016/j.abrep.2020.100255
2. Sprenger S, Anderson JS. Dying to Quit: Understanding the Burden of Tobacco in Psychiatric Patients-A Clinical Review. J Psychiatr Pract. 2024 Jan 1;30(1):23-31. doi: 10.1097/PRA.0000000000000764. PMID: 38227724.
3. Prochaska JJ, Gill P, Hall SM. Treatment of Tobacco Use in an Inpatient Psychiatric Setting. PS. 2004;55(11):1265-1270. doi:10.1176/appi.ps.55.11.1265
4. Garakani A, Appel JM, Aloysi AS, Martinez JM, Larkin K, Buono FD. Patient Requests for Discharge from Voluntary Psychiatric Hospitalization: a Chart Review. Psychiatr Q. 2019;90(4):849-859. doi:10.1007/s11126-019-09671-y
Methods: A retrospective analysis was conducted using a random sample of adult patients admitted voluntarily to inpatient psychiatric facilities in a nationwide hospital system. Exclusionary criteria included medical discharge, administration of electroconvulsive therapy, hospital stay > 29 days, and patients with indeterminate demographics or smoking status. Demographic variables including age, sex, race, insurance type, and psychiatric diagnosis were assembled. Binary logistic regression with a Firth correction was used to determine associations between patient directed discharge (PDD) rates and smoking status, smoking cessation treatments, demographic variables, comorbidities, and use patterns.
Results: A total of 30,000 patients were randomly sampled resulting in 25,829 patients after the application of exclusionary criteria. The average age in the sample was 41 years (SD=17.3) and 54.5% of patients smoked with an average use of 1.18 packs per day (SD=1.5). Smoking status was significantly associated with the likelihood of PDD (χ2 = 49.42, p < 0.0001, OR = 2.16). This effect was preserved despite controlling for other variables (χ2 = 21.50, p < 0.0001 OR = 1.74). Pharmaceutical intervention overall was associated with a decreased PDD (χ2 = 4.43, p < 0.05 OR = 1.29), however nicotine replacement therapy (NRT) alone had a significant association (χ2 = 8.16, p < 0.01 OR 1.42). Bupropion and varenicline were not associated with significant differences in PDD rates. Rates of PDD remained elevated despite treatment relative to patients who did not smoke (χ2 = 22.02, p < 0.0001, OR = 1.86). Sex (χ2 = 4.77, p < 0.05) was significantly associated with discharge rates while racial identity and insurance type were significant only when comparing Hispanic to White (χ2 = 4.68, p < 0.05) and Medicaid to no insurance (χ2 = 6.41, p < 0.05). Interestingly, use characteristics including packs per day, pack years, use of smokeless tobacco, and use of vapes were not significantly associated with likelihood of PDD (all p > 0.05). Co-occurring substance use disorder (SUD) was associated with elevated risk of PDD (χ2 = 16.76, p < 0.0001, OR 1.62) while diagnoses of depression (χ2 = 17.48, p < 0.0001, OR = 0.62), psychosis (χ2 = 48.98, p < 0.0001, OR = 0.36), and bipolar disorder (χ2 = 22.60, p < 0.0001, OR = 0.52) were associated with decreased risk.
Conclusion & Discussion: This was the largest study of its kind investigating the association between tobacco use and patient directed discharge rates in a national sample of psychiatric patients. The results support previous findings that more than half of psychiatric inpatients report smoking and use of tobacco is associated with increased risk of PDD while providing further insight on the effect of pharmacotherapy. This was the first attempt to investigate the association of PDD with individual treatment modalities. NRT alone was associated with lower PDD rates while bupropion and varenicline were not. Contrary to previous reports, the risk of PDD remained significantly elevated despite treatment. Sex and co-occurring SUD were associated with higher risk while other demographic variables were not. The finding that use characteristics including duration and amount of smoking was not associated with PDD rates is querulous and warrants replication. Tobacco cessation constitutes an important aspect of psychiatric care and consistent use of NRT may attenuate but not normalize the risk of PDD for patients who smoke.
References: 1. Kagabo R, Gordon AJ, Okuyemi K. Smoking cessation in inpatient psychiatry treatment facilities: A review. Addict Behav Rep. 2020;11:100255. doi:10.1016/j.abrep.2020.100255
2. Sprenger S, Anderson JS. Dying to Quit: Understanding the Burden of Tobacco in Psychiatric Patients-A Clinical Review. J Psychiatr Pract. 2024 Jan 1;30(1):23-31. doi: 10.1097/PRA.0000000000000764. PMID: 38227724.
3. Prochaska JJ, Gill P, Hall SM. Treatment of Tobacco Use in an Inpatient Psychiatric Setting. PS. 2004;55(11):1265-1270. doi:10.1176/appi.ps.55.11.1265
4. Garakani A, Appel JM, Aloysi AS, Martinez JM, Larkin K, Buono FD. Patient Requests for Discharge from Voluntary Psychiatric Hospitalization: a Chart Review. Psychiatr Q. 2019;90(4):849-859. doi:10.1007/s11126-019-09671-y
Learning Objectives:
- Describe the prevalence of smoking in psychiatric inpatients and understand the association with negative treatment outcomes including patient directed discharge rates.
- Appreciate the risk factors for patient directed discharge rates in psychiatric inpatients who smoke specifically sex and cooccurring substance use disorder.
- Understand the association between pharmacotherapy and patient directed discharge rates in psychiatric inpatients who smoke and to stratify the interventions most helpful to attenuating the risk.
