Neurocognitive disorder and exposure to medication for opioid use disorder
(28) Neurocognitive Disorder and Exposure to Medication for Opioid Use Disorder
Friday, April 5, 2024
9:45 AM - 1:15 PM
Has Audio

Molly M. Perri, MD
Resident Physician
University of Chicago Hospitals, Illinois
Andrea J. Landi, MD
Assistant Professor
University of Chicago, Illinois
Presenter(s)
Background & Introduction: The rate of opioid-related overdose deaths has quadrupled since 2002 among adults age 65 and older (Humphreys & Shover, 2023). There is undeniable evidence that harm reduction strategies, specifically the three FDA-approved medications for opioid use disorder (MOUD), reduce mortality for people with opioid use disorder (OUD) (Volkow et al., 2014). Though OUD is a growing health problem in older adults, MOUD is severely underutilized. A cross-sectional study from 2022 revealed only 13% of adults age 50 and older with OUD reported use of MOUD in the past year (Mauro et al., 2022). In addition to OUD-related complications, older adults also face a higher prevalence of age-related conditions and chronic disease, specifically dementia. Therefore, it is imperative to address the unique needs at the intersection of OUD and aging. There is no research evaluating the impact that neurocognitive disorders have on patients’ ability to participate in MOUD treatment. The primary objective of our retrospective chart review was to investigate the association between neurocognitive disorder and exposure to MOUD in older adults age 65 and older.
Methods: A retrospective chart review was conducted of patients age 65 and older with a diagnosis of OUD who received primary care services at an academic medical center in Chicago, Illinois from January 2018 to June 2022. All charts with a diagnosis of OUD were considered for inclusion. Charts were excluded if the patient did not have an active diagnosis of OUD (OUD in remission or only opioid dependence without a use disorder) or if the patient’s chart was inactive during the study period. All patient charts were evaluated for demographic data, substance use characterization, geriatric syndromes (including neurocognitive disorder), healthcare utilization, and MOUD exposure. Exposure to MOUD was defined as at least one day of MOUD use during the study window. A Pearson Chi-Square test was used to assess for a statistically significant association between neurocognitive disorder and MOUD exposure. An independent t-test was used to compare the average duration on MOUD during the study period between patients with neurocognitive disorder and those without it. The study period for each patient was defined by the first and last date within the study window where the patient had an office visit, ER visit, or hospital admission.
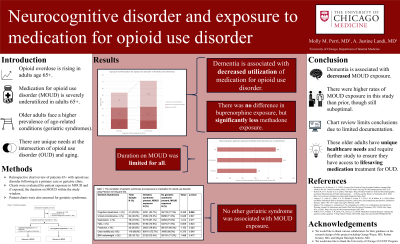
Results: A total of 327 charts were considered for inclusion and of those, 167 were excluded due to chart inactivity (n = 8) or no active diagnosis of OUD (n = 163). Of the 160 charts included, 41 patients (25.6%) had a diagnosis of neurocognitive disorder. Patients with neurocognitive disorder were found to have less exposure to MOUD (22/41, 53.6%) than those without neurocognitive disorder (92/119, 77.3%; p = .004). Exposure to buprenorphine was not significantly different between the groups, however, exposure to methadone was less frequent in patients with neurocognitive disorder (15/41, 36.6%) than those without neurocognitive disorder (68/119, 57.1%; p = .023). The average duration on MOUD during the study window was significantly lower for patients with neurocognitive disorder (M = 31%, SD .42) than those without it (M = 51%, SD = .44; p = .015). No other geriatric syndrome (urinary incontinence, depression, falls, fractures, mobility aid use, or underweight BMI) showed significant association to MOUD exposure between patients with and without neurocognitive disorder.
Conclusion & Discussion: Patients age 65 and older with OUD who have a neurocognitive disorder are poorly characterized in the literature. Our retrospective chart review found that patients age 65 and older with OUD and a diagnosis of neurocognitive disorder have significantly less exposure to MOUD compared to those without neurocognitive disorder. This study population had high rates of exposure to MOUD compared to prior studies, however, these patients were actively followed in a primary care clinic having frequent healthcare engagement. Additionally, though exposure was high, the number of days on MOUD was limited for both patients with neurocognitive disorder and without. This study is limited by data collection being completed through chart review as providers may have incomplete documentation and methadone prescription history is not freely available in the electronic medical record. Older adults with co-occurring diagnoses of OUD and neurocognitive disorder are a population that has unique healthcare needs and requires further study to ensure they have access to lifesaving medication treatment for OUD.
References: Humphreys, K., & Shover, C. L. (2023). Twenty-Year Trends in Drug Overdose Fatalities Among Older Adults in the US. JAMA Psychiatry, 80(5), 518-520. https://doi.org/10.1001/jamapsychiatry.2022.5159
Kariisa M, D. N., Kumar S, et al. (2022). Vital Signs: Drug Overdose Deaths, by Selected Sociodemographic and Social Determinants of Health Characteristics — 25 States and the District of Columbia, 2019–2020. https://www.cdc.gov/vitalsigns/overdose-death-disparities/index.html
Lennon, J. C., Aita, S. L., Bene, V. A. D., Rhoads, T., Resch, Z. J., Eloi, J. M., & Walker, K. A. (2022). Black and White individuals differ in dementia prevalence, risk factors, and symptomatic presentation. Alzheimers Dement, 18(8), 1461-1471. https://doi.org/10.1002/alz.12509
Mauro, P. M., Gutkind, S., Annunziato, E. M., & Samples, H. (2022). Use of Medication for Opioid Use Disorder Among US Adolescents and Adults With Need for Opioid Treatment, 2019. JAMA Netw Open, 5(3), e223821. https://doi.org/10.1001/jamanetworkopen.2022.3821
Volkow, N. D., Frieden, T. R., Hyde, P. S., & Cha, S. S. (2014). Medication-assisted therapies--tackling the opioid-overdose epidemic. N Engl J Med, 370(22), 2063-2066. https://doi.org/10.1056/NEJMp1402780
Methods: A retrospective chart review was conducted of patients age 65 and older with a diagnosis of OUD who received primary care services at an academic medical center in Chicago, Illinois from January 2018 to June 2022. All charts with a diagnosis of OUD were considered for inclusion. Charts were excluded if the patient did not have an active diagnosis of OUD (OUD in remission or only opioid dependence without a use disorder) or if the patient’s chart was inactive during the study period. All patient charts were evaluated for demographic data, substance use characterization, geriatric syndromes (including neurocognitive disorder), healthcare utilization, and MOUD exposure. Exposure to MOUD was defined as at least one day of MOUD use during the study window. A Pearson Chi-Square test was used to assess for a statistically significant association between neurocognitive disorder and MOUD exposure. An independent t-test was used to compare the average duration on MOUD during the study period between patients with neurocognitive disorder and those without it. The study period for each patient was defined by the first and last date within the study window where the patient had an office visit, ER visit, or hospital admission.
Results: A total of 327 charts were considered for inclusion and of those, 167 were excluded due to chart inactivity (n = 8) or no active diagnosis of OUD (n = 163). Of the 160 charts included, 41 patients (25.6%) had a diagnosis of neurocognitive disorder. Patients with neurocognitive disorder were found to have less exposure to MOUD (22/41, 53.6%) than those without neurocognitive disorder (92/119, 77.3%; p = .004). Exposure to buprenorphine was not significantly different between the groups, however, exposure to methadone was less frequent in patients with neurocognitive disorder (15/41, 36.6%) than those without neurocognitive disorder (68/119, 57.1%; p = .023). The average duration on MOUD during the study window was significantly lower for patients with neurocognitive disorder (M = 31%, SD .42) than those without it (M = 51%, SD = .44; p = .015). No other geriatric syndrome (urinary incontinence, depression, falls, fractures, mobility aid use, or underweight BMI) showed significant association to MOUD exposure between patients with and without neurocognitive disorder.
Conclusion & Discussion: Patients age 65 and older with OUD who have a neurocognitive disorder are poorly characterized in the literature. Our retrospective chart review found that patients age 65 and older with OUD and a diagnosis of neurocognitive disorder have significantly less exposure to MOUD compared to those without neurocognitive disorder. This study population had high rates of exposure to MOUD compared to prior studies, however, these patients were actively followed in a primary care clinic having frequent healthcare engagement. Additionally, though exposure was high, the number of days on MOUD was limited for both patients with neurocognitive disorder and without. This study is limited by data collection being completed through chart review as providers may have incomplete documentation and methadone prescription history is not freely available in the electronic medical record. Older adults with co-occurring diagnoses of OUD and neurocognitive disorder are a population that has unique healthcare needs and requires further study to ensure they have access to lifesaving medication treatment for OUD.
References: Humphreys, K., & Shover, C. L. (2023). Twenty-Year Trends in Drug Overdose Fatalities Among Older Adults in the US. JAMA Psychiatry, 80(5), 518-520. https://doi.org/10.1001/jamapsychiatry.2022.5159
Kariisa M, D. N., Kumar S, et al. (2022). Vital Signs: Drug Overdose Deaths, by Selected Sociodemographic and Social Determinants of Health Characteristics — 25 States and the District of Columbia, 2019–2020. https://www.cdc.gov/vitalsigns/overdose-death-disparities/index.html
Lennon, J. C., Aita, S. L., Bene, V. A. D., Rhoads, T., Resch, Z. J., Eloi, J. M., & Walker, K. A. (2022). Black and White individuals differ in dementia prevalence, risk factors, and symptomatic presentation. Alzheimers Dement, 18(8), 1461-1471. https://doi.org/10.1002/alz.12509
Mauro, P. M., Gutkind, S., Annunziato, E. M., & Samples, H. (2022). Use of Medication for Opioid Use Disorder Among US Adolescents and Adults With Need for Opioid Treatment, 2019. JAMA Netw Open, 5(3), e223821. https://doi.org/10.1001/jamanetworkopen.2022.3821
Volkow, N. D., Frieden, T. R., Hyde, P. S., & Cha, S. S. (2014). Medication-assisted therapies--tackling the opioid-overdose epidemic. N Engl J Med, 370(22), 2063-2066. https://doi.org/10.1056/NEJMp1402780
Learning Objectives:
- Upon completion, participants will be able to describe the association between dementia and MOUD exposure.
- Upon completion, participants will be able to explain the unique healthcare considerations for patients with OUD and neurocognitive disorder.
- Upon completion, participants will be able to describe the risk of limited screening and treatment for older adults with OUD and dementia.
