(60) Buprenorphine Dose and Dosing Frequency Must Be Increased During Pregnancy
Saturday, April 6, 2024
9:45 AM - 1:15 PM
Has Audio

Raman Venkataramanan, PhD
Professor
University of Pittsburgh, Pennsylvania- SC
Steve Caritis, MD
Professor
University of Pittsburgh, Pennsylvania
Presenter(s)
Non-presenting author(s)
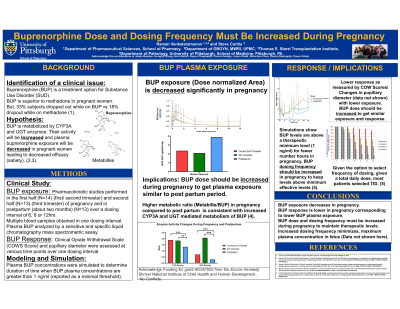
Background & Introduction: Buprenorphine along with methadone is used for treatment of substance use disorder during pregnancy. Buprenorphine dosing in pregnancy is currently based on dosing schemes in non-pregnant subjects. This has led to a significant lack of adherence to buprenorphine in pregnant women. A previous study in a small number of subjects from our group has shown that pregnancy increases the clearance and decreases the plasma exposure of buprenorphine. The right way to increase buprenorphine exposure has not been clearly documented previously. The aim of this research is to further validate the impact of pregnancy on buprenorphine exposure at various trimesters with clinical observations and computational approaches; and to evaluate the impact of increasing dose and dosing frequency on maintaining buprenorphine plasma concentration above the minimum therapeutic concentration of 1 ng/ml.
Methods: We designed a clinical study to evaluate the pharmacokinetics of buprenorphine during first, second and third trimester of pregnancy. Blood samples were obtained at various time points during a dosing interval, and plasma was obtained immediately by centrifugation at room temperature. A sensitive (Limit of quantification of 0.05 ng/ml) and specific high pressure liquid chromatographic method was used to measure the concentration of buprenorphine and three of its metabolites. Non-compartmental analysis was performed to calculate the dose normalized area under the plasma concentration vs time (AUC) (a marker of drug exposure), during the early part and late part of pregnancy in comparison to the postpartum period. ANOVA was used to determine the significance of the differemces observed.
We also performed a population pharmacokinetic analysis to identify pregnancy as a covariate contributing to the differences in dose normalized AUC. We applied physiologically based pharmacokinetic modeling to determine the impact of various trimesters of pregnancy on dose normalized AUC. We performed additional modeling and simulations to evaluate the impact of differing doses and dosing intervals on the maximum and minimum plasma concentration obtained during pregnancy. Pupillary diameter was also measured multiple times in a dosing interval.
Results: The dose normalized AUC was 2.4, 2.1 and 3.9 ng/ml/hr, during 1/2 trimester, 3rd trimester and postpartum (n=36), clearly documenting increased clearance and decreased exposure to BUP in pregnancy. The decrease in buprenorphine exposure was consistent with the increase in buprenorphine metabolites to parent buprenorphine AUC ratios. They were 1.89, 1.84, and 1.33 for the demethylated metabolite, and 0.71, 2.07, and 0.3 for the conjugated metabolite during 1/2 trimester, 3rd trimester and postpartum, respectively. Correspondingly, at least a minimum of 50% increase in dose is necessary to have comparable AUC in pregnancy.
In population pharmacokinetic analysis pregnancy was identified as a covariate impacting buprenorphine exposure. With modeling approach we could document increase in clearance of buprenorphine in first trimester itself.
Among the 14 women participating in the pharmacokinetic study during and after pregnancy, plasma concentrations of buprenorphine were < 1 ng/mL (the theoretical concentration required to prevent withdrawal symptoms) for 50-80% of the 12 hour dosing interval while at steady state. In 62 women in a opioid agonist treatment program, in which dosing frequency is determined in part by patient preference, 16% were on once-daily dosing, 16% were on twice-daily dosing, 45% were on thrice-daily dosing, and 23% were on four-times-daily dosing. With further computer simulations, for the 6mg daily dose, mean plasma concentrations exceed the 1 ng/ml threshold for the first 7.7 hours, but the concentrations were lower than 1 ng/ml for the rest of the 24 hour study period i.e. 16.3 hours. With the 3mg BID dose, plasma concentrations are below 1ng/ml for a total of 14.4 hours. With the 2 mg TID dosing interval, mean concentrations are below 1ng/ml for a total of 10.8 hours in a day. Plasma concentrations with the TID regimen are below the 1 ng/ml threshold for a shorter length of time than other dosing regimens.
With a lower buprenorphine plasma AUC, the response to buprenorphine (pupillary diameter change) was also lower during pregnancy.
Conclusion & Discussion: 1. Buprenorphine exposure is decreased in pregnancy.
2. The lower exposure was associated with lower response to buprenorphine.
3. Increased dose and dosing frequencies are necessary to maintain comparable plasma exposure (AUC) during pregnancy and postpartum and to obtain proper response.
4. For a given daily dose, increasing the dosing frequency will maintain the plasma concentration above the threshold of 1 ng/ml for a longer duration in a day.
Our study population is limited to predominantly white subjects due to the population democraphics in our center. Future studies should be performed in an expanded subject population.
References: 1: Zhang H, Bastian JR, Zhao W, Chen H, Shaik IH, Chaphekar N, Caritis SN, Venkataramanan R. Pregnancy Alters CYP- and UGT-Mediated Metabolism of Buprenorphine. Ther Drug Monit. 2020 Apr;42(2):264-270. doi: 10.1097/FTD.0000000000000724. PMID: 31929398; PMCID: PMC9082566.
2: Bastian JR, Chen H, Zhang H, Rothenberger S, Tarter R, English D, Venkataramanan R, Caritis SN. Dose-adjusted plasma concentrations of sublingual buprenorphine are lower during than after pregnancy. Am J Obstet Gynecol. 2017 Jan;216(1):64.e1-64.e7. doi: 10.1016/j.ajog.2016.09.095. Epub 2016 Sep 26. PMID: 27687214; PMCID: PMC5245872.
3: Caritis SN, Bastian JR, Zhang H, Kalluri H, English D, England M, Bobby S, Venkataramanan R. An evidence-based recommendation to increase the dosing frequency of buprenorphine during pregnancy. Am J Obstet Gynecol. 2017 Oct;217(4):459.e1-459.e6. doi: 10.1016/j.ajog.2017.06.029. Epub 2017 Jun 29. PMID: 28669739; PMCID: PMC5614874.
4: Zhang H, Kalluri HV, Bastian JR, Chen H, Alshabi A, Caritis SN, Venkataramanan R. Gestational changes in buprenorphine exposure: A physiologically-based pharmacokinetic analysis. Br J Clin Pharmacol. 2018 Sep;84(9):2075-2087. doi: 10.1111/bcp.13642. Epub 2018 Jun 21. PMID: 29873094; PMCID: PMC6089832.
Methods: We designed a clinical study to evaluate the pharmacokinetics of buprenorphine during first, second and third trimester of pregnancy. Blood samples were obtained at various time points during a dosing interval, and plasma was obtained immediately by centrifugation at room temperature. A sensitive (Limit of quantification of 0.05 ng/ml) and specific high pressure liquid chromatographic method was used to measure the concentration of buprenorphine and three of its metabolites. Non-compartmental analysis was performed to calculate the dose normalized area under the plasma concentration vs time (AUC) (a marker of drug exposure), during the early part and late part of pregnancy in comparison to the postpartum period. ANOVA was used to determine the significance of the differemces observed.
We also performed a population pharmacokinetic analysis to identify pregnancy as a covariate contributing to the differences in dose normalized AUC. We applied physiologically based pharmacokinetic modeling to determine the impact of various trimesters of pregnancy on dose normalized AUC. We performed additional modeling and simulations to evaluate the impact of differing doses and dosing intervals on the maximum and minimum plasma concentration obtained during pregnancy. Pupillary diameter was also measured multiple times in a dosing interval.
Results: The dose normalized AUC was 2.4, 2.1 and 3.9 ng/ml/hr, during 1/2 trimester, 3rd trimester and postpartum (n=36), clearly documenting increased clearance and decreased exposure to BUP in pregnancy. The decrease in buprenorphine exposure was consistent with the increase in buprenorphine metabolites to parent buprenorphine AUC ratios. They were 1.89, 1.84, and 1.33 for the demethylated metabolite, and 0.71, 2.07, and 0.3 for the conjugated metabolite during 1/2 trimester, 3rd trimester and postpartum, respectively. Correspondingly, at least a minimum of 50% increase in dose is necessary to have comparable AUC in pregnancy.
In population pharmacokinetic analysis pregnancy was identified as a covariate impacting buprenorphine exposure. With modeling approach we could document increase in clearance of buprenorphine in first trimester itself.
Among the 14 women participating in the pharmacokinetic study during and after pregnancy, plasma concentrations of buprenorphine were < 1 ng/mL (the theoretical concentration required to prevent withdrawal symptoms) for 50-80% of the 12 hour dosing interval while at steady state. In 62 women in a opioid agonist treatment program, in which dosing frequency is determined in part by patient preference, 16% were on once-daily dosing, 16% were on twice-daily dosing, 45% were on thrice-daily dosing, and 23% were on four-times-daily dosing. With further computer simulations, for the 6mg daily dose, mean plasma concentrations exceed the 1 ng/ml threshold for the first 7.7 hours, but the concentrations were lower than 1 ng/ml for the rest of the 24 hour study period i.e. 16.3 hours. With the 3mg BID dose, plasma concentrations are below 1ng/ml for a total of 14.4 hours. With the 2 mg TID dosing interval, mean concentrations are below 1ng/ml for a total of 10.8 hours in a day. Plasma concentrations with the TID regimen are below the 1 ng/ml threshold for a shorter length of time than other dosing regimens.
With a lower buprenorphine plasma AUC, the response to buprenorphine (pupillary diameter change) was also lower during pregnancy.
Conclusion & Discussion: 1. Buprenorphine exposure is decreased in pregnancy.
2. The lower exposure was associated with lower response to buprenorphine.
3. Increased dose and dosing frequencies are necessary to maintain comparable plasma exposure (AUC) during pregnancy and postpartum and to obtain proper response.
4. For a given daily dose, increasing the dosing frequency will maintain the plasma concentration above the threshold of 1 ng/ml for a longer duration in a day.
Our study population is limited to predominantly white subjects due to the population democraphics in our center. Future studies should be performed in an expanded subject population.
References: 1: Zhang H, Bastian JR, Zhao W, Chen H, Shaik IH, Chaphekar N, Caritis SN, Venkataramanan R. Pregnancy Alters CYP- and UGT-Mediated Metabolism of Buprenorphine. Ther Drug Monit. 2020 Apr;42(2):264-270. doi: 10.1097/FTD.0000000000000724. PMID: 31929398; PMCID: PMC9082566.
2: Bastian JR, Chen H, Zhang H, Rothenberger S, Tarter R, English D, Venkataramanan R, Caritis SN. Dose-adjusted plasma concentrations of sublingual buprenorphine are lower during than after pregnancy. Am J Obstet Gynecol. 2017 Jan;216(1):64.e1-64.e7. doi: 10.1016/j.ajog.2016.09.095. Epub 2016 Sep 26. PMID: 27687214; PMCID: PMC5245872.
3: Caritis SN, Bastian JR, Zhang H, Kalluri H, English D, England M, Bobby S, Venkataramanan R. An evidence-based recommendation to increase the dosing frequency of buprenorphine during pregnancy. Am J Obstet Gynecol. 2017 Oct;217(4):459.e1-459.e6. doi: 10.1016/j.ajog.2017.06.029. Epub 2017 Jun 29. PMID: 28669739; PMCID: PMC5614874.
4: Zhang H, Kalluri HV, Bastian JR, Chen H, Alshabi A, Caritis SN, Venkataramanan R. Gestational changes in buprenorphine exposure: A physiologically-based pharmacokinetic analysis. Br J Clin Pharmacol. 2018 Sep;84(9):2075-2087. doi: 10.1111/bcp.13642. Epub 2018 Jun 21. PMID: 29873094; PMCID: PMC6089832.
Learning Objectives:
- Describe/Articulate the need for increased dose and dosing frequency of buprenorphine during pregnancy.
- Compare various approaches used to establish novel dosing regimen for drugs used to treat substance use disorder in special patient populations.
- Update practice guidelines in regards to the use of medications to treat substance use disorder during pregnancy.
