(57) Stuck in a Ketamine Use Cycle: Anxiety, Cystitis, and Pain
Saturday, April 6, 2024
9:45 AM - 1:15 PM
Has Audio

Yonina Mar, MD
Addiction Medicine Attending Physician, Assistant Clinical Professor
Mount Sinai Health System, New York
Presenter(s)
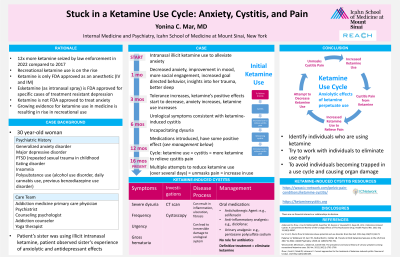
Background & Introduction: According to a May 2023 study in JAMA Psychiatry, law enforcement agencies seized more than 1,500 pounds of ketamine in 2022, which was approximately 12 times more than in 2017. The growing body of evidence for the use of ketamine in treatment-resistant depression, anxiety, schizophrenia, substance use disorders, and chronic pain has had a significant impact on increasing rates of recreational use. Despite its promising results, ketamine has also been shown to serve as a reinforcing stimulus to induce self-administration in rats, suggesting its high potential for abuse in humans. With both acute and chronic ketamine use, toxic systemic effects can ensue. Chronic ketamine use can lead to significant urinary system complications including ketamine-induced cystitis in which individuals struggle with symptoms of severe dysuria, frequency, urgency, and gross hematuria. Inflammation, ulceration, and fibrosis can lead to irreversible damage to the urological system. Oral treatments for pain and inflammation can improve symptoms, however they are often unable to achieve significant and durable effects, and more invasive treatments are required. As ketamine is an anesthetic, it can serve to alleviate these symptoms that it ultimately causes, thus perpetuating use and maintaining a use cycle, making it difficult for individuals to eliminate use.
Case Description: V is a 30 year-old woman with a history of generalized anxiety disorder, major depressive disorder, PTSD (repeated sexual trauma in childhood), eating disorder, insomnia and polysubstance use. She began using illicit intranasal ketamine after observing the anxiolytic and antidepressant effects that her sister experienced with illicit ketamine use. Within a month of starting use, V began experiencing increases in positive mood, social engagement, goal-directed behavior (e.g., attending events, going on trips, discussing volunteer opportunities) and insights into the effect of her trauma on her difficulty functioning in her 20s. By three months, her tolerance had increased, and her use did not have the same alleviating effects on anxiety, mood, and insomnia. By six months, urological symptoms consistent with ketamine-induced cystitis became prominent and dysuria became incapacitating. She entered into a cycle of using more ketamine for its analgesic properties to alleviate the urological pain that was ultimately caused by the ketamine use. Her attempts to reduce her ketamine use unmasked the urological pain, which led to an increase in use to counteract the pain. Medications to manage urinary symptoms were started with some positive effects. Her team of providers including an addiction medicine primary care physician, a psychiatrist, a psychologist, an addiction counselor, and a yoga therapist continue to work collaboratively to help V manage her anxiety, depression, and ketamine use using a trauma-informed and harm reduction approach. She continues to struggle with ongoing ketamine use, which is perpetuated by its mild alleviation of anxiety and depressive symptoms, but mostly to avoid the urological pain that is unmasked when ketamine use decreases or is eliminated. Ketamine has become both physically and psychologically alleviating and exacerbating and has seized V in a vicious cycle of ongoing use.
Conclusion & Discussion: Recreational ketamine use is rapidly rising and it is important for the medical community to be aware of the detrimental toxic effects it can have on organ systems, in particular the urological system. Though ketamine is the culprit of deleterious urinary effects, its anesthetic effects can act to counteract these symptoms and maintain a dysfunctional and perpetuating use cycle. This case illustrates the difficulty in breaking this cycle and eliminating ketamine use. It is important to identify individuals at risk of ketamine abuse and try and eliminate use early in order to avoid patients becoming trapped in a use cycle and causing organ damage.
References: 1. Zhou J, Scott C, Miab ZR, Lehmann C. Current approaches for the treatment of ketamine-induced cystitis. Neurourol Urodyn. 2023 Mar;42(3):680-689.
2. Liu Y, Lin D, Wu B, Zhou W. Ketamine abuse potential and use disorder. Brain Res Bull. 2016 Sep;126(Pt 1):68-73.
3. Winstock AR, Mitcheson L, Gillatt DA, Cottrell AM. The prevalence and natural history of urinary symptoms among recreational ketamine users. BJU Int. 2012;110(11):1762‐1766.
Case Description: V is a 30 year-old woman with a history of generalized anxiety disorder, major depressive disorder, PTSD (repeated sexual trauma in childhood), eating disorder, insomnia and polysubstance use. She began using illicit intranasal ketamine after observing the anxiolytic and antidepressant effects that her sister experienced with illicit ketamine use. Within a month of starting use, V began experiencing increases in positive mood, social engagement, goal-directed behavior (e.g., attending events, going on trips, discussing volunteer opportunities) and insights into the effect of her trauma on her difficulty functioning in her 20s. By three months, her tolerance had increased, and her use did not have the same alleviating effects on anxiety, mood, and insomnia. By six months, urological symptoms consistent with ketamine-induced cystitis became prominent and dysuria became incapacitating. She entered into a cycle of using more ketamine for its analgesic properties to alleviate the urological pain that was ultimately caused by the ketamine use. Her attempts to reduce her ketamine use unmasked the urological pain, which led to an increase in use to counteract the pain. Medications to manage urinary symptoms were started with some positive effects. Her team of providers including an addiction medicine primary care physician, a psychiatrist, a psychologist, an addiction counselor, and a yoga therapist continue to work collaboratively to help V manage her anxiety, depression, and ketamine use using a trauma-informed and harm reduction approach. She continues to struggle with ongoing ketamine use, which is perpetuated by its mild alleviation of anxiety and depressive symptoms, but mostly to avoid the urological pain that is unmasked when ketamine use decreases or is eliminated. Ketamine has become both physically and psychologically alleviating and exacerbating and has seized V in a vicious cycle of ongoing use.
Conclusion & Discussion: Recreational ketamine use is rapidly rising and it is important for the medical community to be aware of the detrimental toxic effects it can have on organ systems, in particular the urological system. Though ketamine is the culprit of deleterious urinary effects, its anesthetic effects can act to counteract these symptoms and maintain a dysfunctional and perpetuating use cycle. This case illustrates the difficulty in breaking this cycle and eliminating ketamine use. It is important to identify individuals at risk of ketamine abuse and try and eliminate use early in order to avoid patients becoming trapped in a use cycle and causing organ damage.
References: 1. Zhou J, Scott C, Miab ZR, Lehmann C. Current approaches for the treatment of ketamine-induced cystitis. Neurourol Urodyn. 2023 Mar;42(3):680-689.
2. Liu Y, Lin D, Wu B, Zhou W. Ketamine abuse potential and use disorder. Brain Res Bull. 2016 Sep;126(Pt 1):68-73.
3. Winstock AR, Mitcheson L, Gillatt DA, Cottrell AM. The prevalence and natural history of urinary symptoms among recreational ketamine users. BJU Int. 2012;110(11):1762‐1766.
Learning Objectives:
- describe the effects of ketamine, its misuse potential, and the risks for developing ketamine use disorder.
- describe the disease process of ketamine-induced cystitis.
- describe a management plan for ketamine-induced cystitis, including medications that can help alleviate symptoms and a strategy for helping to eliminate use.
