(91) Factors Predicting MOUD Access for (Un)housed Patients: A Machine Learning Approach
Saturday, April 6, 2024
9:45 AM - 1:15 PM
Has Audio
- AE
Aaron Esguerra
Medical Student
Michigan State University College of Human Medicine, Michigan 
Thomas J. Weinandy, PhD
Research Economist
Upside, Michigan
Presenter(s)
Non-presenting author(s)
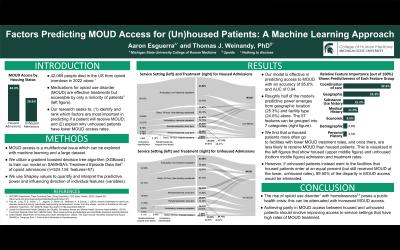
Background & Introduction: Opioid use disorder (OUD) is a growing public health emergency, with opioids involved in 81.8% of all overdose deaths in the United States. Treatment via medications for opioid use disorder (MOUD) (e.g., methadone, buprenorphine, naltrexone) is an effective therapeutic approach, and can thus lower the risk of death from overdose. Despite this, only 22.1% of individuals with OUD report receiving these medications. Multiple factors influence access to MOUD. Homelessness is a notable barrier, associated with limited resources and support, a higher prevalence of physical and psychiatric comorbidities, and an unstable surrounding milieu; homelessness is also linked to increased rates of opioid overdose. Machine learning, compared to traditional statistical methods, provides closer examination of the nuance and interactions between influencing factors, especially for large data sets; no study has employed this approach to explain the discrepancy in MOUD access between housed and unhoused patients. Our study seeks to add to the literature by leveraging a machine learning approach to answer two research questions. First, we quantitatively evaluate and rank the factors that predict MOUD access for all patients with OUD. Second, we measure the discrepancies in MOUD access by housing status and identify the source of the disparity.
Methods: We utilize a gradient boosted decision tree algorithm to train our model to predict whether a patient receives MOUD. We use the Substance Abuse and Mental Health Services Administration’s Treatment Episode Data Set-Admissions, which contains 524,134 opioid admissions to treatment facilities across the United States, and reports numerous demographic and clinical features for each individual admission; we incorporate these features into the 57 variables in our model. We then use Shapley values to quantify and interpret the predictive power and influencing direction of individual variables (i.e., determine their feature importance).
Results: There are 44.92% of opioid admissions from patients who live independently receiving MOUD, while only 28.56% of unhoused admissions receive MOUD. Our trained model is 85.55% accurate at predicting MOUD outcome and has an area under the ROC curve of 0.9383, indicating strong reliability. The four geographic features of the service setting admitting a patient together contribute 25.34% toward the model’s predictive power, and the service setting itself contributes 24.03%. Combined, this means that nearly half of the model’s prediction is determined before a patient even walks through the door. Other features with relatively higher importance include the referral source (6.87%), a patient’s history of prior treatment (4.13%), and their frequency of opioid use (3.58%).
Since Shapley values are assigned to each feature for each observation, we can also compare the magnitude and direction of these Shapley values for subgroups within a given feature. For example, admissions from patients living independently have a median Shapley value of 0.06, indicating that their living status most often predicts they will receive MOUD. Conversely, unhoused admissions have a median Shapley value of -0.07 associated with their living status, indicating they are less likely to receive MOUD. These values show how the model has “learned” a pattern in the data, suggesting an association between housing status and differential MOUD access.
Finally, we consider the role of service setting in predicting MOUD access. We find that unhoused admissions are disproportionately likely to be in certain service settings compared to independent living admissions, and once there, those unhoused admissions are often less likely to receive MOUD than their independent living counterparts. In fact, if homeless patients were admitted to service settings in the same way independent living patients were, their MOUD treatment rates would increase from 28.56% to 43.20%. This counterfactual alone would eliminate 89.50% of the disparity in MOUD access between homeless and independent living admissions.
Conclusion & Discussion: This study demonstrates the utility of a machine learning model that predicts MOUD access and both ranks the influencing variables and compares their individual positive or negative contribution to access. One application is to apply the model on individual patients to estimate their probability of receiving treatment and then personalize care based on their at-risk factors. Another application is our insight that the best way to improve MOUD access for the unhoused population is to better connect patients to service settings that are more likely to offer MOUD.
One limitation of using Shapley values is how their relative values will change as variables are added or removed from a model. Although we intentionally use a dataset that is large in features and observations, future research could consider whether new information about a patient or facility will change our results. We also find “what” predicts MOUD access, but further research should explore “how” to expand unhoused patient access to service settings that offer MOUD.
References: Hsu, M., Jung, O. S., Kwan, L. T., Jegede, O., Martin, B., Malhotra, A., & Suzuki, J. (2024). Access challenges to opioid use disorder treatment among individuals experiencing homelessness: Voices from the streets. Journal of Substance Use and Addiction Treatment, 157, 209216.
Kong, Y., Zhou, J., Zheng, Z., Amaro, H., & Guerrero, E. G. (2022). Using machine learning to advance disparities research: Subgroup analyses of access to opioid treatment. Health Services Research, 57(2), 411–421.
McLaughlin, M. F., Li, R., Carrero, N. D., Bain, P. A., & Chatterjee, A. (2021). Opioid use disorder treatment for people experiencing homelessness: A scoping review. Drug and Alcohol Dependence, 224, 108717.
Wadekar, A. S. (2020). Understanding Opioid Use Disorder (OUD) using tree-based classifiers. Drug and Alcohol Dependence, 208, 107839.
Warren, D., Marashi, A., Siddiqui, A., Eijaz, A. A., Pradhan, P., Lim, D., Call, G., & Dras, M. (2022). Using machine learning to study the effect of medication adherence in Opioid Use Disorder. PLOS ONE, 17(12), e0278988.
Methods: We utilize a gradient boosted decision tree algorithm to train our model to predict whether a patient receives MOUD. We use the Substance Abuse and Mental Health Services Administration’s Treatment Episode Data Set-Admissions, which contains 524,134 opioid admissions to treatment facilities across the United States, and reports numerous demographic and clinical features for each individual admission; we incorporate these features into the 57 variables in our model. We then use Shapley values to quantify and interpret the predictive power and influencing direction of individual variables (i.e., determine their feature importance).
Results: There are 44.92% of opioid admissions from patients who live independently receiving MOUD, while only 28.56% of unhoused admissions receive MOUD. Our trained model is 85.55% accurate at predicting MOUD outcome and has an area under the ROC curve of 0.9383, indicating strong reliability. The four geographic features of the service setting admitting a patient together contribute 25.34% toward the model’s predictive power, and the service setting itself contributes 24.03%. Combined, this means that nearly half of the model’s prediction is determined before a patient even walks through the door. Other features with relatively higher importance include the referral source (6.87%), a patient’s history of prior treatment (4.13%), and their frequency of opioid use (3.58%).
Since Shapley values are assigned to each feature for each observation, we can also compare the magnitude and direction of these Shapley values for subgroups within a given feature. For example, admissions from patients living independently have a median Shapley value of 0.06, indicating that their living status most often predicts they will receive MOUD. Conversely, unhoused admissions have a median Shapley value of -0.07 associated with their living status, indicating they are less likely to receive MOUD. These values show how the model has “learned” a pattern in the data, suggesting an association between housing status and differential MOUD access.
Finally, we consider the role of service setting in predicting MOUD access. We find that unhoused admissions are disproportionately likely to be in certain service settings compared to independent living admissions, and once there, those unhoused admissions are often less likely to receive MOUD than their independent living counterparts. In fact, if homeless patients were admitted to service settings in the same way independent living patients were, their MOUD treatment rates would increase from 28.56% to 43.20%. This counterfactual alone would eliminate 89.50% of the disparity in MOUD access between homeless and independent living admissions.
Conclusion & Discussion: This study demonstrates the utility of a machine learning model that predicts MOUD access and both ranks the influencing variables and compares their individual positive or negative contribution to access. One application is to apply the model on individual patients to estimate their probability of receiving treatment and then personalize care based on their at-risk factors. Another application is our insight that the best way to improve MOUD access for the unhoused population is to better connect patients to service settings that are more likely to offer MOUD.
One limitation of using Shapley values is how their relative values will change as variables are added or removed from a model. Although we intentionally use a dataset that is large in features and observations, future research could consider whether new information about a patient or facility will change our results. We also find “what” predicts MOUD access, but further research should explore “how” to expand unhoused patient access to service settings that offer MOUD.
References: Hsu, M., Jung, O. S., Kwan, L. T., Jegede, O., Martin, B., Malhotra, A., & Suzuki, J. (2024). Access challenges to opioid use disorder treatment among individuals experiencing homelessness: Voices from the streets. Journal of Substance Use and Addiction Treatment, 157, 209216.
Kong, Y., Zhou, J., Zheng, Z., Amaro, H., & Guerrero, E. G. (2022). Using machine learning to advance disparities research: Subgroup analyses of access to opioid treatment. Health Services Research, 57(2), 411–421.
McLaughlin, M. F., Li, R., Carrero, N. D., Bain, P. A., & Chatterjee, A. (2021). Opioid use disorder treatment for people experiencing homelessness: A scoping review. Drug and Alcohol Dependence, 224, 108717.
Wadekar, A. S. (2020). Understanding Opioid Use Disorder (OUD) using tree-based classifiers. Drug and Alcohol Dependence, 208, 107839.
Warren, D., Marashi, A., Siddiqui, A., Eijaz, A. A., Pradhan, P., Lim, D., Call, G., & Dras, M. (2022). Using machine learning to study the effect of medication adherence in Opioid Use Disorder. PLOS ONE, 17(12), e0278988.
Learning Objectives:
- Upon completion, participant will be able to articulate the discrepancy in access to medications for opioid use disorder (MOUD) between housed and unhoused patients.
- Upon completion, participant will be able to describe machine learning as a tool used to predict whether a patient with opioid use disorder receives MOUD
- Upon completion, participant will be able to identify service setting/facility as a major reason behind the discrepancy in MOUD access between housed and unhoused patients.
